Accelerate Access. Elevate STARs. Reduce Avoidable Costs.
Ensure every member transitions home with timely, high-quality services—and elevate their care experience with ongoing, proactive support in the home.

How Dina Serves Medicare Advantage Plans
Vendor Network Management
Accelerated Access to Care
STARs Improvement via Transitions of Care
Used By Innovative Health Plans and Providers






***This field does NOT display
Improved Start-of-Care Times
“We are seeing improvements in several areas: start-of-care timeframes, provider communication, efficiency, and employee morale.”
Kirah Simonian
Director, Referral Management tango

See How We Help Medicare Advantage Plans Drive Results
Position your plan to exceed member expectations, boost Star Ratings and offload significant administrative burden. Schedule a discovery call today.
Seamlessly Extend CM & UM Systems
Disconnected data, manual documentation, and workflow silos are among the top reasons Medicare Advantage plans struggle to hit quality and cost targets. Streamline coordination and transition care programs with Dina’s API-based platform and network designed to seamlessly integrate and extend your existing platforms.
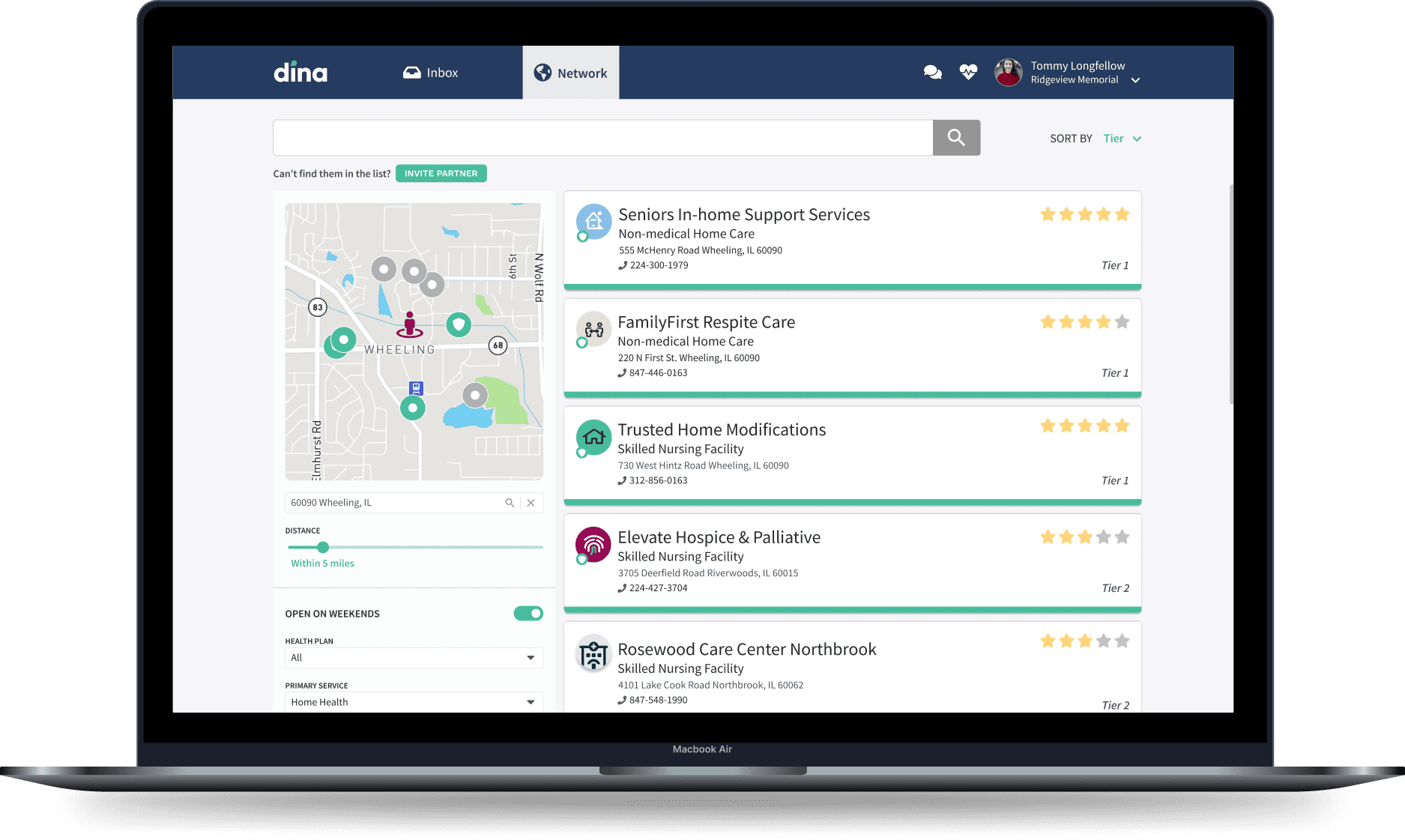

Actually Streamlining Coordination
We’ve heard that coordinators and care managers are overworked, spend time finding availability and chasing documents, vendor partners struggle to effectively participate, and that members ultimately suffer. We’ve seen DIY tools, manual workflows, and other platforms try to solve the problem. Dina is here to partner with you and bring order to the chaos. We engage vendors, automate unnecessary tasks, and optimizes your network for continued success. We give your teams’ time back while making your members happier and healthier.
More from Team Dina!

Case Manager Leans on “Patchwork Quilt” of Services to Address Social Determinant Issues
Colleen Morley on backing her team, coaching family caregivers, treating social determinants, and increasing patient education. Case managers are often referred to as patient advocates. Colleen Morley is a self-described “advocate of the advocates.” She is the...

Here’s How Northwestern Medicine Earned $700,000 in Bundled Reimbursements
Three Northwestern Medicine hospitals in suburban Illinois were paying CMS penalties averaging $300,000 a year. One challenge: preventing its bundled payment patients from making a U-turn back into the hospital. To combat this issue, the hospital wanted to help its...
How to Use Data to Become a Preferred Provider
When hospitals select preferred providers, they often rely on skilled nursing facilities or home health agencies that they’ve built relationships with and trust. Providers may be friends or long-time partners. Or, they might bring in lunch or treats for hospital...
