%
Faster Start of Care
%
Visit Documents Collected
Minutes to Confirm Availability
Caseload Improvement
How We Help
Provider Identification
Contracting & Credentialing
Service Coordination
Visit Notes Collection
Reconciliation & Payments
Performance Management
Who We Serve
PACE Programs
Special Needs Plans
Medicare Advantage
Modernizing Network Management of In-Home Services
Traditional network management for in-home services is operationally expensive, unresponsive, and ill-adapted to serve the unique needs of care managers, product designers, and the current network management team.
From provider identification to contracting and credentialing, Dina simplifies, organizes, and aligns your approach to in-home service network management with key outcomes and performance milestones. Leveraging Agentic AI, in-home care contracting experts, and Dina’s fulfillment platform, we reduce administrative expenses while significantly streamlining critical access to outcome improving personal care services.
Used by Leading Government Programs





Faster Access = Better Outcomes
Mins to Confirm Services
Days to Launch
%
Fewer ER Visits
Administrative ROI
%
Fewer Hospitalizations
Network Partners
Services Coordinated
%
Uptime

Reduce Costly
Healthcare Moments
To reduce costly healthcare moments like readmissions, avoidable hospitalizations, and ED visits, Dina’s contracted network of caregiver agencies and fulfillment platform leads to accelerated starts of care by finding the right provider for the right member.
We pair quality-oriented, SLA-backed networks with closed loop coordination powered by proprietary data sources to ensure members are supported at key moments in their journey.
News & Insights
Learn more about connecting to one of today’s
most important care settings: the home.

Integrated Home Care Services Acquires Dina, Creating the Category-Defining Platform for In-Home Benefit Management
Combination pairs Integrated’s decades of specialized home care benefit management expertise and value-based operational scale with Dina’s AI-powered orchestration to make care in the home more effective, simple, and affordable for all. MIRAMAR, FL, MAY 20, 2026...
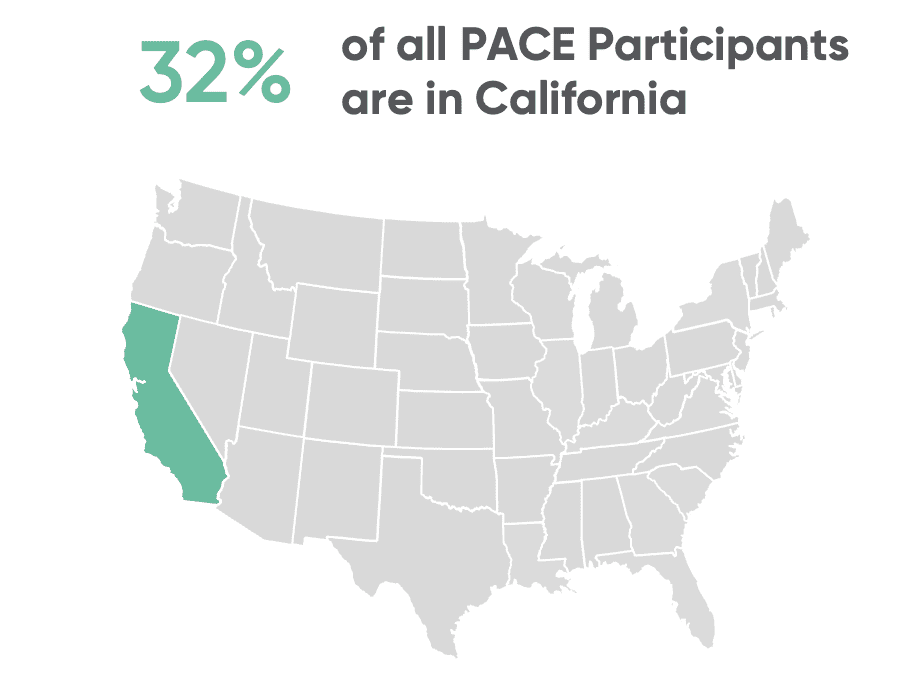
PACE Began in California. Its Next Chapter May Be Defined There.
California’s Program of All‑Inclusive Care for the Elderly (PACE) is entering a pivotal moment. Across the United States, demand for community‑based care models is accelerating as the population ages and policymakers search for alternatives to institutional care. PACE...

Closing the Gap Between SNP Design and Delivery: Operationalizing In-Home Care for 2027
As Medicare Advantage product teams finalize their 2027 bids, the pressure is on. Decisions made now will shape not only benefit design, but also the operational complexity plans will live with for years to come. For teams designing Special Needs Plans (SNPs), one...

Dina Recognized as Finalist for the 2025 Digital Health Awards at HLTH
Chicago, IL, October 6, 2025 — Dina, is thrilled to announce its selection as a finalist for the prestigious 2025 Digital Health Hub Foundation: Digital Health Awards at HLTH. Dina was chosen as a finalist for the Rising Star - Home Health Diagnostic &...
2025 in Review — What California Health Plans Need to Prepare for in 2026 and 2027
As 2025 comes to a close, California health plans are reflecting on a year defined by regulatory changes, budget pressures, and growing demands for better care coordination, integration, and dual-eligibility management. The challenge has been clear: serve more complex...

The OBBBA has Arrived: Navigating Policy Shifts Driving Special Needs Plans Forward
The One Big Beautiful Bill Act (OBBBA) is more than just sweeping federal legislation—it marks a decisive shift in how dual-eligible care will be financed and delivered. While headlines have focused on tax reforms and political infighting, two foundational provisions...
